Research Group Andrée
Tissue Engineering
Using tissue engineering, implants will be developed for the reconstruction or replacement of damaged organs. For this purpose, biological matrices and tissue-type-specific primary cells are used. The optimal replacement of diseased or damaged tissue (e.g. heart valves, vessels, vascular valves) is performed with autologous (patient-own) cells seeded on a matrix. At present, laboratory research focuses on cell and development biology, as well as on cell culture engineering. With currently available biomedical technologies, form and function of the bioartificial tissue will be "prefabricated" in vitro in a bioreactor. Subsequently, vital tissue will be implanted into patients to reach its final stability and full function in vivo, following maturation within the recipient’s body. The use of autologous cells from the implant recipient should:
- minimize the danger of rejection,
- make the use of immunosuppressive drugs unnecessary,
- exclude the transmission of infection agents,
- ensure the ability of the implant to grow in step with the patient (eg. in the case of children)
Heart Valves and Blood Vessels
The overall goal of currently running projects is to use tissue engineering technology to create autologous heart valves (pulmonary valves, aortal valves and mitral valves) and large diameter blood vessels (aorta and valved veins). The prosthetic materials being developed must have the following properties to be suitable for clinical application.
- They must be autologous, i.e. non-immunogenic.
- They must be antithrombogenic.
- They must be capable of growth during normal development of the recipient.
The basic scaffold material is obtained from allogenic or xenogenic vessels which can be decellularized without damage to the connective tissue matrix, so that it can be subsequently repopulated with a prospective recipient’s own endothelial cells. The engineered tissues being produced are tested in large animal models.
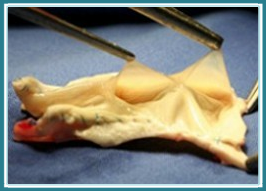
Vascularized Trachea Replacements
At present, there is no suitable material for repairing tracheae damaged by tumor removal or trauma or for the surgical correction of birth defects of the airway. This deficiency calls for a bioartificial solution and promising tracheal replacements are currently being constructed from autogenous sections of small intestine obtained with an intact blood supply. These are stabilized by the attachment of cartilage bracing to the outer surface and a layer of autologous epithelial cells is then grown on the inner surface prior to use.
Vascularized Myocardial Patches
There is an intensive worldwide research effort to improve the treatment of acute cardiac infarct. One approach is to inject stem cells from a variety of different sources directly into a recent infarct with the expectation that factors introduced by or with these stem cells will prevent the death of the cardiomyocytes stressed by anoxia, or alternatively, that differentiation of the injected stem cells will produce replacement cardiomyocytes. An alternative approach involves the production of bioengineered replacement tissue to repair myocardial damage which has occurred days or even weeks in the past. For this purpose, both cultured heart muscle tissue and vascularized myocardial patches are being implanted into fibrotic myocardial scar tissue. Both, small and large animal models are used for testing the practicality of this alternative approach.