Achalasia
Achalasia is a functional disorder of the smooth muscles of hollow organs that perform a closing function due to a lack of relaxation (reduction in tone) of the muscles. Achalasia of the esophagus is a rare motor disorder of the lower part of the esophagus in children, in which there is a lack of relaxation of the lower esophageal sphincter muscle (esophageal sphincter) with resulting narrowing. The part of the esophagus that lies above this is therefore dilated and sluggish (hypoperistaltic).
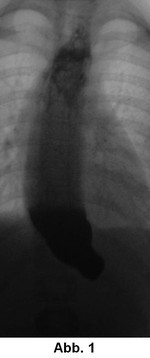
Achalasia is caused by pathologically altered nerve cells in the muscular wall of the esophagus. The children are usually characterized by insufficient food intake, vomiting of undigested food and failure to thrive. Achalasia is diagnosed by means of an X-ray open-swallow examination, which shows the narrowing of the lower part of the esophagus and widening of the upper part of the esophagus (Fig. 1). By measuring the pressure in different sections of the oesophagus (oesophageal manometry), a zone of increased tension in the oesophageal muscles (so-called high pressure zone) can be detected. An endoscopy of the oesophagus may reveal a build-up of food residue above the achalasia or signs of oesophageal inflammation caused by refluxed stomach acid.
Since drug therapies, dilatations and the injection of drugs into the esophageal sphincter have not become established, surgical therapy is the method of choice. The principle is to cut through all muscle layers of the lower oesophagus including the transition to the stomach (cardia) while preserving the mucous membrane (mucosa). This surgical method is called "esophagomyotomy according to Heller".
Initial contact is always made by means of an outpatient consultation in our pediatric surgery outpatient clinic (see below for contact details). The treatment options will be presented and your questions will be discussed in detail. Please bring all existing examination results with you to the first outpatient information meeting.
However, additional examinations are often necessary, some of which can be carried out close to home:
24 h pH-metry (acid measurement)
In this examination, a very thin cable with 2 measuring sensors is placed through the nose into your child's esophagus. A portable device connected to this measures the pH value, i.e. the acidity, at the lower end of the probe at two measuring points. If acidic gastric juice flows back into the oesophagus, the pH value changes. This allows you to see how long and how often the gastric juice has been rising. However, this method does not provide any information about damage to the mucous membrane of the esophagus or the lungs.
(X-ray) pulp swallowing examination
This examination is not carried out to detect reflux, but to detect malformations or diseases that promote reflux (e.g. a diaphragmatic hernia or "hiatal hernia"). In the case of achalasia, there is a narrowing of the lower part of the oesophagus and a widening of the upper part of the oesophagus.
Gastroscopy (gastroscopy or oesophagogastroduodenoscopy ("ÖGD"))
In individual cases, it may be necessary to perform an esophagoscopy and gastroscopy in order to determine whether the mucous membrane of the esophagus has been damaged. Under general anesthesia, a flexible tube with a camera attached to it is inserted into the esophagus and stomach. If inflamed mucous membrane is seen, tiny samples can be taken from the mucous membrane with small forceps and examined.
"Heller esophagomyotomy" or Heller myotomy
This operation is always performed laparoscopically at our center, regardless of age. The pediatric surgeon makes a small incision in the navel through which a thin tube (trocar) is inserted into the abdominal cavity. Air is blown into the abdominal cavity through the trocar and a camera is inserted (laparoscopy). This allows the entire abdomen to be inspected. Additional working channels (trocars) are then inserted into the abdomen via two or three further 3 mm incisions. During the Heller myotomy, the musculature of the esophagus including the first part of the stomach (cardia) is incised and spread over a distance of approx. 5 cm (Fig. 2-6). Previous bougienage is not a contraindication for this procedure. There is agreement that a so-called fundoplication is performed in the same session (the esophagus is wrapped around with parts of the stomach like a cuff to create a valve mechanism) (Fig. 7). This is intended to prevent acidic gastric juice from flowing back into the esophagus (gastroesophageal reflux). The inertia or "motor disturbance" of the esophagus remains after the myotomy and can become problematic in the long term. For this reason, and because of the possibility of recurrence (return of the same clinical symptoms), children who have undergone myotomy should be subject to an annual follow-up program. A recurrence of achalasia can also be successfully treated with minimally invasive surgery.
After the procedure, your child will initially remain in the recovery area, where you will be able to sit up in bed again. You will then be transferred to the normal ward. A few hours after the operation, your child will usually be able to eat again. A 3-4 day stay in hospital is usually sufficient for a Heller myotomy.
Conservative therapy
We do not carry out drug therapy with a so-called "calcium antagonist" (active ingredient: nifedipine), pharmacological-interventional therapy by injecting botulinum toxin (a neurotoxin) or endoscopic dilation of the esophagus (bougienage) in our Clinical Department, as their long-term effect has not been proven. Surgical therapy is therefore the method of choice.
A follow-up visit to us is only planned after a few weeks. As we only use stitches that dissolve by themselves, the first post-operative check-ups will be carried out by your pediatrician after discharge. However, if any questions remain unanswered or if we consider an earlier follow-up examination to be appropriate in individual cases, you can come back to us at any time.